Living with constant jaw tension, clicking sounds, or chronic headaches can drain your energy and affect your quality of life. Many people spend years managing these symptoms with over the counter painkillers without ever addressing the root cause. If you find it difficult to chew comfortably or wake up with a stiff neck every morning, you are likely searching for effective tmj disorders treatment to find a permanent solution.
The temporomandibular joint is one of the most complex structures in the human body, and when it falls out of alignment, the impact is felt far beyond just your teeth. This guide provides a deep dive into the physiological causes of jaw dysfunction and the modern clinical paths available to restore your health.
You will learn about the latest diagnostic technologies used in 2026 and how a personalized approach can finally stop the cycle of pain.
Understanding TMJ Disorders and Why Professional Care is Vital
The term TMJ refers to the temporomandibular joint, which acts as a sliding hinge connecting your jawbone to your skull. When this joint or the surrounding muscles become inflamed or misaligned, it is classified as a TMJ disorder, often referred to as TMD.
This condition matters because it is rarely an isolated dental issue. It involves a delicate balance between the teeth, the disc within the joint, and the powerful muscles responsible for chewing and speaking.
Ignoring the early signs of dysfunction can lead to long term consequences such as permanent joint damage or severe tooth wear. Because the jaw is closely linked to the nerves in the face and neck, untreated issues often manifest as earaches, dizziness, or migraines. Seeking a professional evaluation ensures that you are treating the mechanical source of the problem rather than just masking the discomfort.
Modern dental science focuses on stabilizing the bite and relaxing the muscular system to achieve lasting results.
Root Causes and Biological Factors Behind Jaw Dysfunction
Understanding why your jaw is hurting is the first step toward successful therapy. Unlike a simple cavity, TMD is often multifactorial, meaning several issues are working together to cause the pain.
Bruxism and Muscular Overuse
Bruxism, or the habitual grinding and clenching of teeth, is a leading contributor to joint strain. Many patients clench their teeth during sleep or high stress situations without realizing it. This constant pressure puts immense stress on the joint capsule and causes the masseter muscles to become hyperactive. Over time, this results in muscle “trigger points” that radiate pain throughout the face and head.
Internal Disc Displacement
Inside your jaw joint sits a small fibrocartilage disc that prevents the bones from rubbing together. In many patients with clicking or popping sounds, this disc has slipped out of its proper position. If the disc is displaced, the joint cannot move smoothly.
This often leads to “locking” where the mouth cannot open or close fully. Real world examples include the sudden inability to take a large bite of food or a sharp catch in the jaw during a yawn.
Occlusal Misalignment and Dental History
Your bite, or how your teeth fit together, dictates how your jaw sits at rest. If your teeth are crowded, missing, or have poorly fitting old dental work, your jaw must shift into an unnatural position to allow the teeth to touch. This constant compensation forces the muscles to work harder and can eventually lead to degenerative changes within the joint itself.
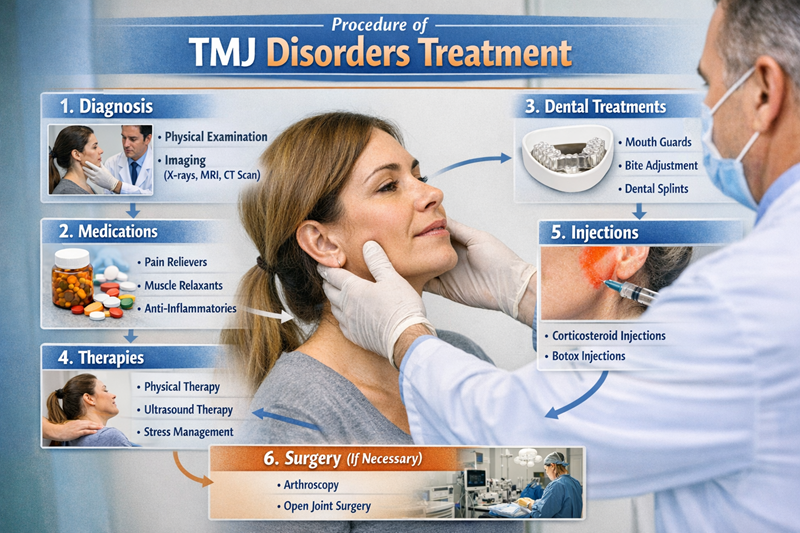
What to Expect During the TMJ Disorders Treatment Process
The path to relief is a structured journey that begins with a comprehensive diagnostic phase. In 2026, we utilize advanced tools to ensure we are not guessing about your health.
- Digital Joint Mapping: We often start with 3D imaging or CBCT scans to view the joint space and the position of the condyles. This allows us to see if there is physical erosion or bone on bone contact.
- Neuromuscular Evaluation: We track how your muscles react when the jaw is in different positions. The goal is to find the “resting position” where your muscles are most relaxed.
- Phase One Stabilization: This usually involves a custom fabricated orthotic or “splint.” Unlike a store bought nightguard, this is a precision medical device designed to hold your jaw in a specific, healthy alignment.
- Trigger Point Therapy: For patients with severe muscle tension, we may use therapeutic injections or ultrasound therapy to “reset” the muscles and allow for immediate relaxation.
- Phase Two Long Term Correction: Once the pain is under control, we look at permanent ways to keep the jaw in that healthy spot. This might include minor dental adjustments, orthodontics, or replacing old crowns that were throwing the bite off.
Common Mistakes to Avoid When Managing Jaw Pain
One of the most frequent errors patients make is relying on “boil and bite” mouthguards from local drugstores. These generic guards are often too soft or poorly fitted, which can actually trigger the brain to chew more frequently during sleep. This increases the activity of the jaw muscles and can make TMJ symptoms significantly worse.
Another mistake is assuming that surgery is the only answer. In reality, the vast majority of cases can be resolved using non invasive, conservative methods like orthotic therapy and lifestyle changes. Patients should also avoid “self adjusting” their bite by grinding their own teeth together or trying to force their jaw to pop.
This physical trauma can cause the internal disc to tear or slip further out of place. Corrective advice involves seeking a professional who uses objective data rather than just physical manipulation.(NIDCR)
Why Local Expertise Matters in Sacramento, Folsom, and Roseville
Seeking treatment close to home in Northern California is essential for the consistent follow up that TMJ therapy requires. Residents of Sacramento, Folsom, and Roseville often lead busy lives that involve long commutes or high stress professional environments, both of which can exacerbate clenching and tension.
Choosing a provider in the Folsom or Roseville area means you can easily attend the routine adjustment appointments necessary for orthotic therapy. Since the jaw is constantly changing as it heals, these small tweaks to your appliance are what ensure the success of the treatment. Furthermore, local providers understand the specific stressors of our community and can offer personalized advice that fits your lifestyle.
When to Speak With a Professional
You should reach out for a consultation the moment you notice that jaw pain is interfering with your daily habits. If you find yourself avoiding certain foods like steak or apples because they are too difficult to chew, your joint is already in distress. Persistent clicking that is accompanied by pain is another clear sign that the internal disc is not functioning correctly.
Trust building in healthcare comes from transparency. You should look for a professional who explains the mechanics of your pain and offers a clear, data driven roadmap for recovery. If you wake up with “tension headaches” more than twice a week, it is highly likely that your jaw is the culprit. Addressing these symptoms early prevents the transition from acute discomfort to a chronic, life altering condition.
Frequently Asked Questions
How long does it take to see results from tmj disorders treatment?
The timeline for relief varies depending on the severity of the joint damage. Most patients begin to feel a significant reduction in muscle tension and headache frequency within the first two to four weeks of wearing a custom orthotic. This initial phase is focused on “decompressing” the joint and allowing the inflammation to subside.
Full stabilization of the joint and the muscles usually takes between three and six months. During this time, your provider will make incremental changes to your appliance to guide the jaw into its most natural and healthy position. It is important to remember that because the muscles have been strained for years, they require time to retrain and stay relaxed.
Will I have to wear a dental appliance forever?
Not necessarily. The goal of phase one therapy is to find the position where your jaw is happy and pain free. Once that position is identified and your symptoms have disappeared, we discuss long term options. Some patients choose to continue wearing a slim, comfortable nightguard to protect their teeth and joint from stress.
Other patients opt for phase two treatment, which involves permanently changing the bite to match the healthy jaw position. This could involve orthodontics or restorative dentistry. The ultimate goal is to give you a smile that functions perfectly on its own without the need for a constant appliance. Your provider will help you choose the path that best fits your goals and budget.
Can stress really cause my jaw joint to fail?
Stress is rarely the sole cause of a TMJ disorder, but it acts as a powerful “accelerant.” When you are under stress, your central nervous system keeps your muscles in a state of high alert. This leads to increased clenching and grinding, which places an enormous physical load on the temporomandibular joint.
If you already have a slight misalignment in your bite, stress provides the extra force needed to push the joint over the edge into painful dysfunction. This is why effective treatment often includes a holistic look at your lifestyle. We focus on physical stabilization of the joint while also providing guidance on how to manage the muscular tension that stress creates.
Speak With an Experienced Specialist Today
Do not let jaw pain dictate your life or limit your ability to enjoy a meal with your family. Living with untreated TMJ issues only leads to more complex problems, including fractured teeth and permanent joint degradation. At our practice serving the Sacramento, Folsom, and Roseville communities, we specialize in the science of neuromuscular dentistry and jaw stabilization.
We use 2026 diagnostic protocols to identify the exact source of your pain and provide a clear, non invasive path to relief. You deserve to wake up without a headache and live a life free from the constant burden of jaw tension. Contact our Folsom office today to schedule your comprehensive evaluation and take the first step toward a healthy, functional smile.